Bangladesh Measles Crisis Reveals Deep Cracks in Public Health System
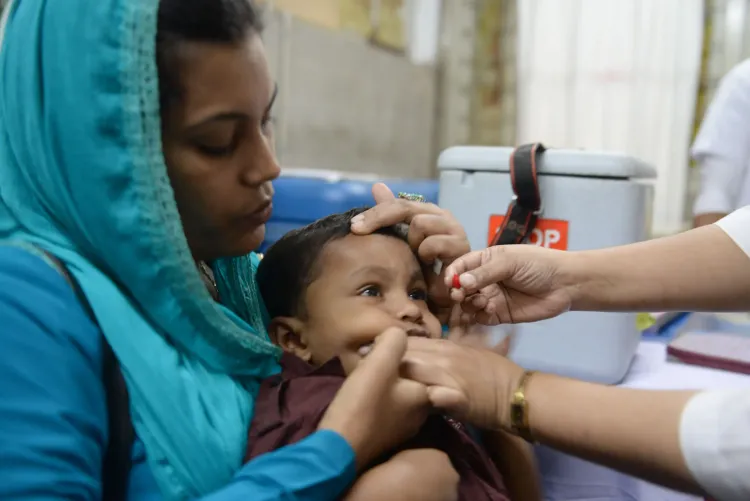
Synopsis
Key Takeaways
Bangladesh's measles vaccine crisis has exposed severe institutional failures within the country's public health infrastructure, with national vaccination coverage collapsing to approximately 60 per cent in 2025 — the lowest level recorded in nearly a decade — down sharply from a consistent 85–92 per cent between 2010 and 2022, according to a detailed report by The Daily Star, Bangladesh's leading English-language newspaper.
A Celebrated Programme Now in Freefall
For years, Bangladesh's Expanded Programme on Immunisation (EPI) stood as one of the country's most admired public health achievements. Backed by sustained government investment, robust development partnerships, and a sprawling network of frontline health workers, the EPI had consistently delivered high vaccination rates while dramatically reducing vaccine-preventable diseases across the South Asian nation.
The programme had long positioned Bangladesh as a model for the developing world. That model, the report now warns, is being systematically dismantled.
"Bangladesh's EPI has long been one of the country's most celebrated public health successes... For years, it positioned the country as a model for the developing world. That model is now being undone," the report stated bluntly.
Governance Failure, Not Just a Logistics Problem
The report is unequivocal that the steep decline in immunisation rates is not a mere supply-chain disruption — it is a fundamental governance failure. Immunisation systems, it explains, depend on predictable, interlocking structures: coordinated procurement, stable financing, functioning leadership, and a reliable frontline workforce. When multiple pillars collapse simultaneously, the entire system breaks down.
A critical policy flashpoint identified in the report is the effective dismantling of the Health, Population and Nutrition Sector Programme (HPNSP) in 2025 — the administrative framework that had governed vaccine procurement for years. Its removal without a credible transition mechanism has been described as a "critical policy failure."
"There is little evidence that this decision was guided by broad technical consultation or risk assessment — an omission that is difficult to justify given the stakes," the report noted.
Vacant Posts and Unpaid Workers Cripple the Cold Chain
Structural weaknesses within the system are equally alarming. The report reveals that nearly 45 per cent of EPI field-level positions across 37 districts remain vacant. These workers are the operational backbone of over 150,000 vaccination centres spread across the country.
Without adequate staffing, coverage declines are not just likely — they are mathematically inevitable. Compounding the crisis, vaccine porters responsible for maintaining the cold chain reportedly went unpaid for several months, triggering widespread unrest and nationwide strikes that further disrupted the delivery of life-saving vaccines to children.
"A system that cannot sustain its frontline workforce cannot sustain its outcomes," the report warned pointedly.
What Must Be Done: The Road to Recovery
The report lays out a clear set of corrective priorities: restore institutional stability, re-establish transparent procurement pathways, urgently fill workforce vacancies, invest in disease surveillance and research, and rebuild public trust through consistent and transparent communication.
Critically, it calls for insulating essential health systems from abrupt policy shifts and administrative discontinuity — a direct reference to the kind of sudden structural changes that triggered the current crisis.
The report draws a stark warning about the cost of inaction: "If addressed now, the broader system stress remains manageable. If not, they will escalate into crises that are far more costly — both financially and in human terms."
Broader Implications: A Warning for South Asia
The Bangladesh measles crisis carries lessons that extend well beyond its borders. Across South Asia, health systems built over decades on international aid, donor partnerships, and government commitment remain vulnerable to sudden policy reversals and funding disruptions. Bangladesh's EPI collapse illustrates how quickly hard-won public health gains can unravel when institutional memory, workforce continuity, and procurement stability are sacrificed in the name of administrative restructuring.
Notably, this crisis unfolds at a time when global measles resurgences have been reported in multiple low- and middle-income countries, partly attributed to COVID-19-era immunisation disruptions that were never fully corrected. Bangladesh's declining coverage makes it increasingly vulnerable to a large-scale measles outbreak — a disease that, while preventable, remains one of the most contagious viruses known to science.
With international health organisations and development partners watching closely, the coming months will determine whether Bangladesh can reverse course before a full-blown epidemic forces a far more expensive and painful reckoning.











